28 October 2023 | Healthcare
The Consumerism Conundrum in Healthcare
By workweek
Healthcare is wonky: it doesn’t operate under free market conditions, making it difficult to have a patient-centric (what I’ll now call ‘consumer-centric’) approach.
In this article, I’ll highlight consumerism in healthcare, explain why consumerizing healthcare is challenging, and share my thoughts on whether healthcare should even be consumerized.
Healthcare Consumerism
Healthcare consumerism empowers patients through more choices, transparent information, and high-quality services. It’s about transforming patients into active consumers who take the driver’s seat in their healthcare decisions, much like they do when making retail or major purchase decisions. Sounds nice!
While incumbent healthcare organizations (e.g. hospitals) are slowly transitioning to the consumer-centric approach to improve the patient experience, digital health and other provider-based startups have taken the reigns on consumerizing healthcare. Companies like Ro, Thirty Madison, Hims & Hers Health have increased consumer access to treatment for common health problems all while maintaining the same level of price transparency as you get from shopping on Amazon. Similarly, Prenuvo and Ezra are two companies offering whole-body imaging scans for anyone who’s willing to pay the (transparent) price. This Twitter exchange sums the above up nicely:
Then we have wearable health tech, which is the epitome of healthcare consumerism, giving patients easy access to their own health data and putting them in control. A recent Deloitte consumer survey found 41% of respondents own a smartwatch or fitness tracker, up from 39% in the previous year. Ninety percent of these folks use wearables to track fitness and monitor health metrics, and 30% of them report these wearables have significantly improved their fitness and health. Most interesting is that 55% of wearable tech users in the survey reported sharing their data with medical providers.

While consumerism in healthcare is a nice beacon to follow, it’s tough to do in the healthcare market.
The Not-So-Free Market
Healthcare consumerism has three qualities that run contrary to the industry’s not-so-free market conditions:
- Transparency: there is a complete lack of clear and accessible information regarding the quality and costs of healthcare services, making informed decisions difficult—if not, impossible.
- Real choice: even if patients have access to information on quality and costs, they don’t have the freedom to choose any provider due to insurance constraints.
- Personal Responsibility: there are an infinite number of societal factors outside of the patient’s control (read: social determinants of health) that impact patients’ health, making it challenging for individuals to fully take charge of their health and subsequent decisions.
To make myself clear: the end-user, or patient, often has little to no information regarding the actual costs they will incur for healthcare services ahead of time. Prices of these services rarely fluctuate in response to the typical forces of supply and demand. Furthermore, a third-party entity (insurance) dictates to the patient-consumer not only which services are accessible but also who is permitted to provide these services. This dynamic significantly restricts consumer choice and transparency, key tenets of a functioning free market and consumerism.
Dash’s Dissection
Healthcare should be consumerized up to a point.
We can consumerize bread-and-butter conditions like acne, hair loss, erectile dysfunction, or sore throat. These prevalent issues come with well-documented, evidence-based treatments that most individuals may need at some point, and physicians/providers have a clear, standardized approach to managing them.
The above is why Amazon launched Amazon Clinic—a direct-to-consumer telehealth marketplace, giving consumers quick access to care options for common conditions without the need for insurance. Prices are known from the get-go. Amazon is essentially placing their healthcare services under free-market conditions (which is what many direct-to-consumer digital health companies do).
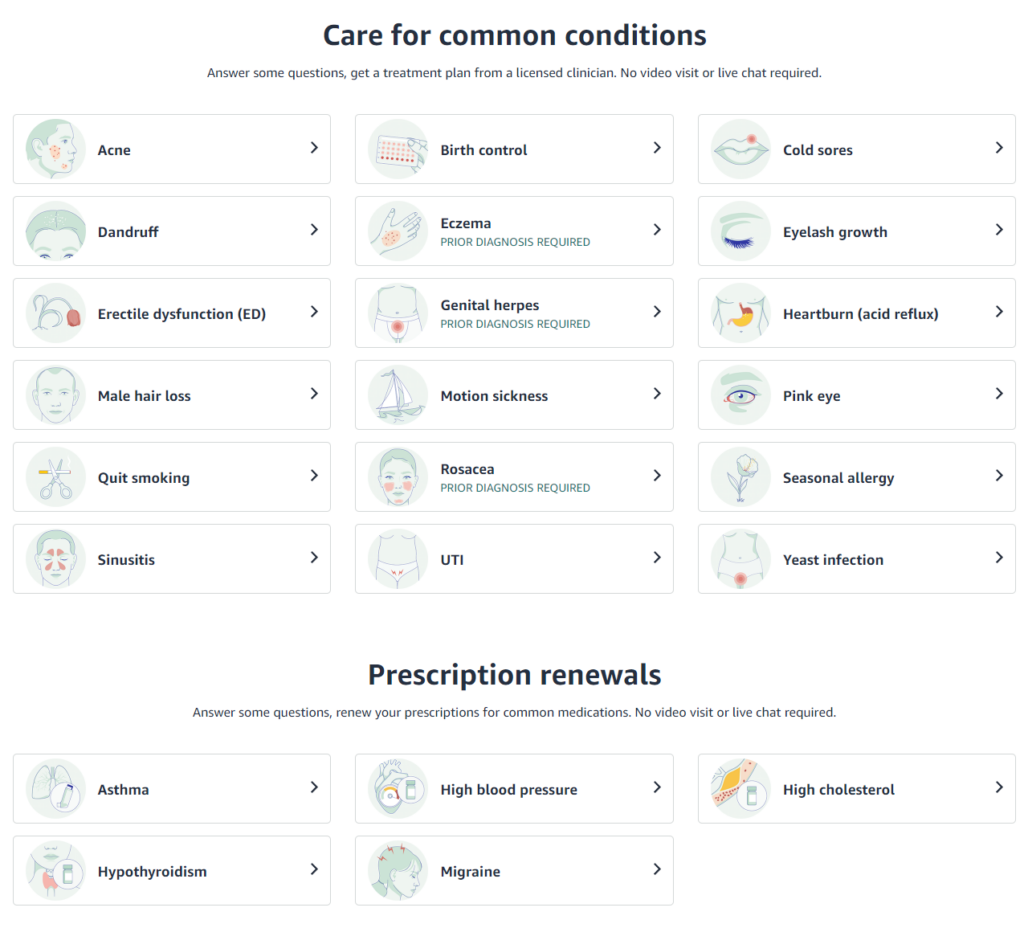
However, when we’re dealing with more complex conditions like cancer, liver disease, autoimmune disorders, and the like, the concept of consumerization becomes murkier and potentially perilous.
These complex conditions warrant thoughtful and tailored care from physicians who use not only the science of medicine to care for patients but the art of medicine. It’s in these intricate cases that the physician-patient relationship becomes paramount, forming the cornerstone of effective care. This relationship, built on trust, empathy, and an in-depth understanding of the patient’s unique health landscape, guides a tailored treatment journey.
Managing these complex conditions is difficult to scale and consumerize (read: it would be challenging to create the “Ro” for liver disease). If they are scaled, it may impact the quality of care and fracture the essential, often fragile bond between physician and patient. This connection is particularly crucial for those navigating the uncertainties and anxieties of serious health issues—which I’m seeing every day in practice. It provides comfort, fosters adherence to often arduous treatment regimens, and encourages the open patient-provider communication necessary for making informed, collaborative decisions.
In summary, while the consumerization of healthcare holds promise for enhancing accessibility and efficiency in certain areas, it is not a one-size-fits-all solution. There are some limitations of a purely consumer-driven approach in contexts requiring the human touch and expertise of physicians.
Stay ahead in healthcare with my weekly Healthcare Huddle newsletter, covering digital health, policy, and business trends for 32,000+ professionals. Share with colleagues and subscribe here.