12 November 2022 | Healthcare
Whole-Body Imaging Scans in Healthy Individuals are Bogus
By workweek
Whole-body imaging scans as a “cancer screening tool” are low-yield in healthy patients with insignificant medical history. If you’re a physician reading this, this isn’t news to you. But if you’re not a physician, don’t be fooled: the benefits of these whole-body scans don’t outweigh the risks, which include unnecessary physical, emotional, and financial harm.
If there are few indications for whole-body scans, why are startups offering these scans popping up across major cities in the U.S.? Because of the money.
In this article, I’ll discuss some startups offering whole-body imaging scans, why these scans are low-value care, and my take on the two last points from a business and provider perspective.
The Deets
Startups offering whole-body imaging scans for healthy individuals are popping up across major cities. While many of these startups exist, I’ll discuss two of them, both of which have similar business models.
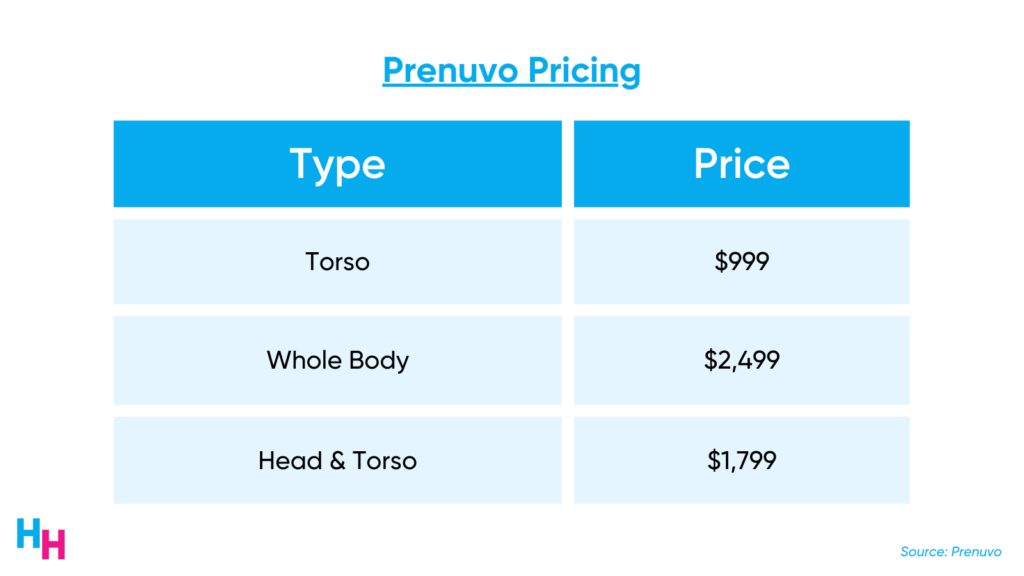
First up is Prenuvo. They offer whole body screening to detect cancer, targeting individuals with unexplained pain, genetic predispositions, or who want “overall peace of mind.”
Rather than wait for symptoms to present and disease to progress, Prenuvo provides early insight into what is going on under the skin.
The company targets patients (primary revenue source) and physicians (primary referral source). Here’s how it works: A physician refers a patient to Prenuvo for a whole body scan; Prenuvo schedules a practitioner consultation to set up the physician’s portal where they can manage referrals and see results; Prenuvo schedules the patient’s scan; Physician and patient receive the final report.
Insurance does not, and likely will never, cover these whole-body imaging scans without any medical indication. The lack of insurance coverage for these scans shouldn’t be a surprise. I could barely get my insurance to approve my MRI indicated for knee pain (for which I’ve had a prior history of a torn meniscus). Insurance won’t even cover an MRI for back pain if the patient doesn’t try NSAIDs or physical therapy first! All this to say, patients using Prenuvo’s services pay out of pocket—straight cash.
Ezra is a similar startup offering whole-body imaging scans for early cancer detection. Just like Prenuvo, physicians can refer patients to Ezra for whole-body imaging scans, track patients’ progress, and receive their reports. But, again, insurance does not cover these scans. Patients must pay out of pocket.
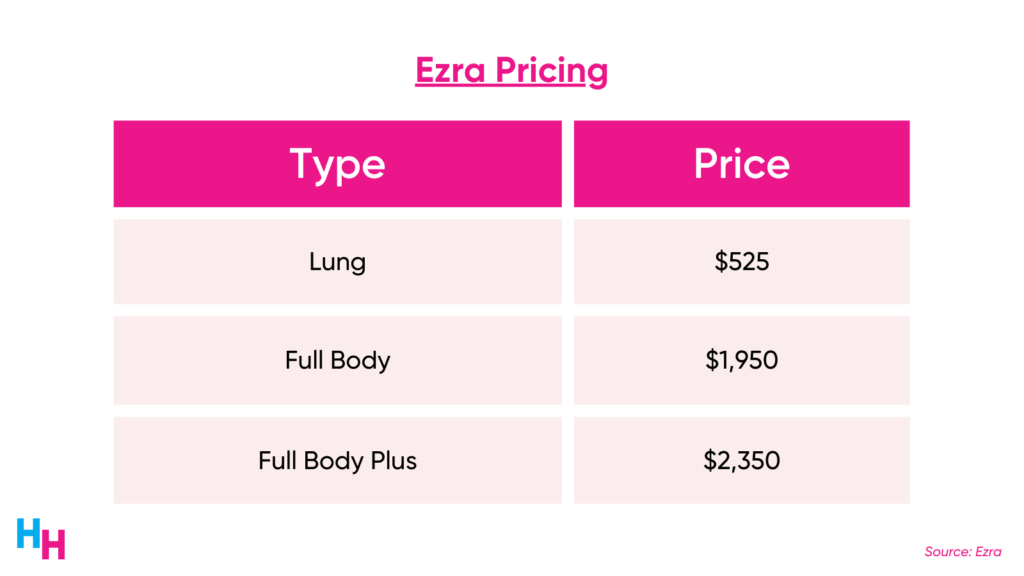
The target market for companies like Prenuvo and Ezra is healthy, upper-class, health-conscious individuals. Hammering this point home: you need over $2,000 in cash to have a whole-body imaging scan. And both companies “recommend” annual scans to maximize the “potential of catching cancer early.” These companies want to keep you coming.
Why You Shouldn’t Get a Whole-Body Scan
There is as much evidence supporting the use of whole-body imaging for cancer screening in healthy individuals as there is evidence supporting that the 2020 election was rigged.
The American College of Preventive Medicine recommends against using whole-body scans for early tumor detection in asymptomatic individuals. There is no evidence suggesting whole-body scans in asymptomatic individuals will improve survival or likelihood of finding tumors, especially since the tumor detection rate is less than 2% in this population.
In one systematic review of whole-body MRI for preventive health screening, the authors found critical and indeterminate incidental findings in asymptomatic subjects were substantial, as were the false positive rates. This review included 12 studies with 5,400 asymptomatic adults without known disease, syndrome, or genetic mutation. The rate of critical and indeterminate incidental findings were both 13% with high variability. The false positive rate was 16%, also with high variability. While people may feel that incidental MRI findings “can save lives,” the authors conclude that physicians should not offer whole-body MRI for preventive health screening to asymptomatic individuals based on current evidence.
The high rates of incidental findings and false positives negatively impact patients’ mental, physical, and financial health:
- Incidental findings increase anxiety in patients.
- Incidental findings may warrant more invasive testing only to yield negative test results.
- Incidental findings that prompt further workup may be increasingly expensive, especially since insurance never approved the whole body scan.
Another review found that abnormal whole-body scan findings are expected in about 95% of individuals. Thirty percent of these individuals would require further investigations, but less than 2% of these findings would actually be reported as suspicious for malignant cancers.
To reiterate, I’m only talking about whole-body scans in asymptomatic individuals with no genetic predispositions. The use of whole-body imaging for cancer screening is indicated and recommended in patients with rare genetic conditions such as Li Fraumeni syndrome and constitutional mismatch repair deficiency. Also, evidence-based preventative scans like mammography are also indicated. But insurance covers these scans.
Dash’s Dissection
If you stare aimlessly at the night sky long enough, you’ll see a shooting star. A shooting star is a meteor 60 miles above the earth’s surface, traveling nearly 30,000 mph. Should you call NASA, freaking out? Probably not. Most meteors are small and disintegrate in the atmosphere. Large meteors that make it through the atmosphere and hit earth are extremely rare.

Similarly, if you scan your whole body without any indication—”staring aimlessly at the sky”— you’re almost certain to find something. And, since this is your body, you’re going to want to find out what that something is, leading to unnecessary anxiety, healthcare procedures, and healthcare spending. This something is highly likely to be a benign incidental finding, meaning you could’ve lived a long and healthy life without knowing of this something. This is essentially why insurance companies would never cover willy-nilly whole-body imaging scans that companies like Prenuvo and Ezra offer.
So, from a medical point of view, there is rarely an indication for a whole-body imaging scan in asymptomatic, healthy individuals. But why are these startups offering these imaging services?
It’s a lucrative business.
An MRI machine costs around $150,000 (not including maintenance). Say Prenuvo purchases one MRI machine. To break even, the company needs to perform one whole-body imaging scan on just one patient on just one-quarter of the annual number of working days. The company is likely performing more than just one scan per day, bringing in millions in annual revenue.
As I stated earlier, the target population is healthy and wealthy individuals who wouldn’t mind dropping $2,000+ on an annual MRI scan. And, these companies are encouraging patients to come back annually to get scanned, likely driving recurring revenue.
In summary, whole-body imaging scans in healthy, asymptomatic individuals are low-value care and not recommended by any physician society. Startups offering whole-body imaging scans as a form of early cancer detection are growing. Despite the futile utility of whole-body scans in a healthy, asymptomatic population to detect cancer, people want to see what’s happening underneath their skin. As such, healthy and wealthy individuals will use the expensive imaging services offered by startups like Prenuvo and Ezra.
If you enjoyed this deep dive, share it with colleagues. Sign up for the Healthcare Huddle newsletter here.