03 April 2022 | Healthcare
Healthcare Q1 ’22 Recap
By workweek
Business
Mark Cuban’s New Pharmacy
Mark Cuban launched an online pharmacy offering common, life-saving medications that are half the price compared to elsewhere. The Mark Cuban Cost Plus Drug Company (MCCPDC) achieves such cost savings by removing health plans and outside middlemen, known as Pharmacy Benefit Managers (PBMs).
How it Works
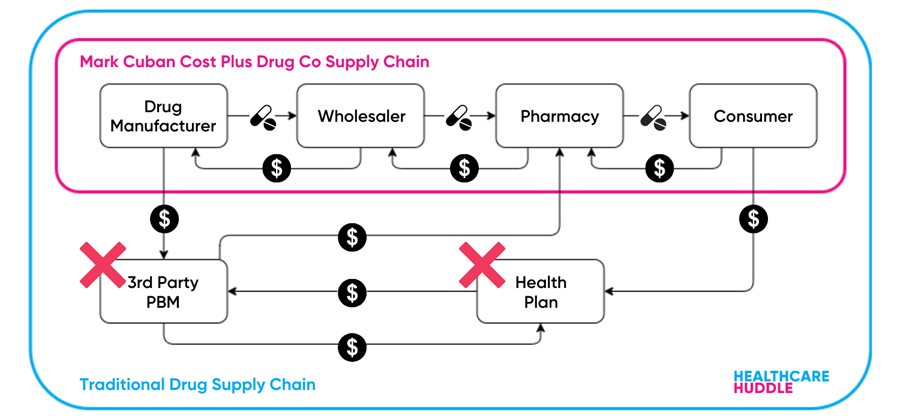
MCCPDC cuts out third-party PBMs by making this a cash-only pharmacy—no health plans allowed. In general, secret negotiations go on in the background of the supply chain between PBMs, health plans, pharmacies and drug manufacturers. These negotiations decide which drugs pharmacies will sell, which drugs health plans will cover and the prices of those drugs. Most importantly, these negotiations decide on the rebates drug manufacturers will pay to PBMs for getting their drugs covered on health plans’ formularies. Negotiations between these players are far from transparent and lead to rising drug prices. So, by cutting out the PBMs you’re also cutting the shady drug pricing negotiations.
Everything else, including drug manufacturer, wholesaler and pharmacy is under one roof, meaning MCCPDC has complete control over its drug supply chain and, therefore, pricing.
The Travel Nursing Saga
The University of Pittsburgh Medical Center (UPMC) is the first medical center to launch an in-house travel nurse staffing agency. The move to in-house will help address nursing shortages and save UPMC money on contracting with outside travel nurse agencies.
Travel Nursing
Pre-pandemic, there were already warnings about a nursing shortage. The shortage certainly became a reality during the pandemic because of severe burnout. In California alone, there’s an estimated shortage of 40,000 nurses. It’s no surprise travel nursing agencies grew 30% in 2020, and likely grew even more in 2021 given the revenue numbers we’re seeing.
Joining a travel nursing agency is quite attractive. These companies may pay 2x-4x the salary nurses are making as hospital employees and allow nurses to choose when they want to work.
Bye.
One-third of nurses plan to leave their jobs by the end of the year, citing burnout and compensation as the main reasons. Staffing firm Incredible Health analyzed hiring data of over 400,000 nurses and surveyed nurses more than 2,500 nurses to see how nurses are faring in year two of the pandemic.
- Incentives. On average, hospitals increased signing bonuses by 162% over the past year, instead of increasing salaries. Texas hospitals, for example, doubled their signing bonuses on average from $5,800 to $10,700 in 2021.
- Travel Nurses. Seventy-seven percent of hospital-employed nurses reported seeing an increase in the number of travel nurses, and one-third reported subsequent culture changes on the floors. Eighty-six percent of hospital-employed nurses cited compensation differences as the leading cause of dissatisfaction with travel nurses.
- The Exodus. One-third of nurses said it’s very likely they quit their role by the end of 2022 because of burnout and poor compensation. Here’s where nurses plan on going after they leave:
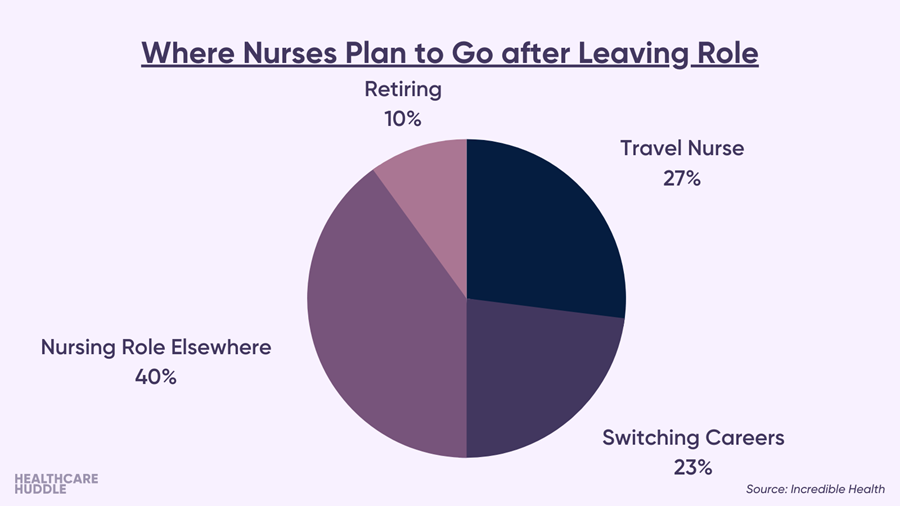
What Can Hospitals Do?
I proposed three actions hospitals can take to address their shortage of nurses:
- Increase their nurses’ salaries to remain competitive with travel nursing agencies.
- Create their own, in-house travel nursing agency as the University Pittsburgh Medical Center did.
- Continue to pay high prices for traveling nurses.
The 2021 Digital Health Funding Skyrockets
A Rock Health report showed digital health funding in 2021 nearly doubled from $14.9 billion to $29.1, the largest year-to-year increase ever.
The Deets
The number of deals in 2021 increased by 50% to 729 deals. 2021 had some of the largest digital health deals ever, with 88 mega deals (over $100 million raised) accounting for 57% of the year’s total funding.
As predicted, digital mental health funding nearly doubled and held its place as the highest-funded digital health sector. Digital mental health also shows no signs of slowing down from the consumer end. While telehealth visits outside of mental healthcare trend towards pre-pandemic levels, telemental health visits are holding steady.
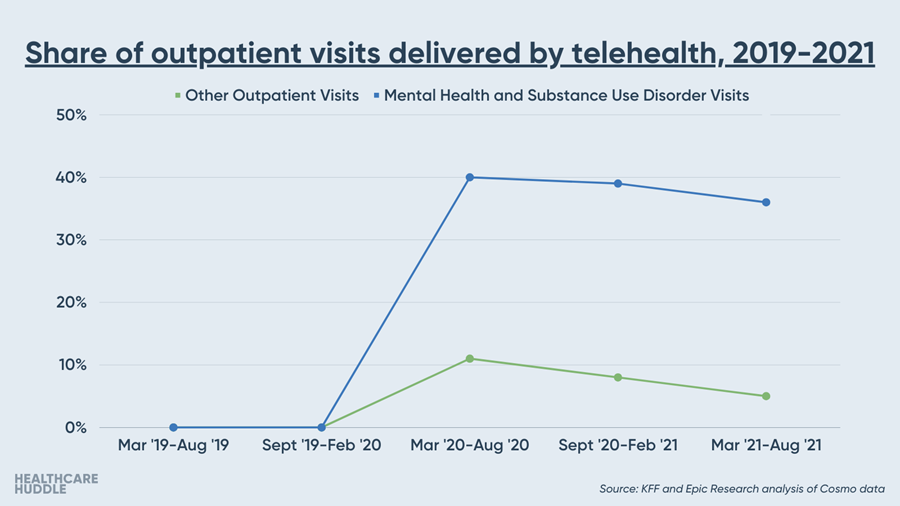
Digital health funding in 2022 may be more significant than in 2021. For example, chronic care management platform Omada Health already raised a whopping $192M in Series E funding this quarter. However, some think 2022 will be the year of consolidation (see below).
Health Tech
Notable Mergers and Acquisitions
- Medical device company Stryker acquired digital communications platform Vocera for $3B. Stryker’s acquisition of Vocera is a step outside of its typical medical device arena but may highlight a new trend of “outsider” companies buying digital health companies.
- Fitness wearable company Withings acquired health and wellness platform 8fit. The acquisition will help Withings compete with strong competitors like Garmin and WHOOP to create personalized data and health plans.
- Specialty care telehealth platform Thirty Madison will merge with women-focused healthcare company Nurx. Through this merger, Thirty Madison will double the number of patients under its care (Nurx is bringing 750k patients) and double the number of conditions the company treats. Thirty Madison looks to be the leading virtual specialty firm in the U.S. The deal’s financial aspects are unknown, but Thirty Madison said it expects to bring in $300M in revenue this year.
- Women’s health platform SimpleHealth acquired competitor contraceptive care company Emme. Through this acquisition, SimpleHealth will expand its contraception delivery and telehealth services to remain competitive against the many players in the women’s health sector.
- In a move that will expand its footprint in the fertility space, online pharmacy Ro acquired male fertility startup Dadi for around $100M. This acquisition rides Ro’s 2021 acquisition of another fertility startup Modern Fertility for $225M.
Insurance
Medicare Advantage Enrollment Soars
Medicare Advantage (MA) plans saw an 8.8% increase in enrollment this year, totaling 28.5 million MA beneficiaries. MA enrollment is growing around 10% per year and the Congressional Budget Office projects the share of MA enrollees will surpass that of Original Medicare beneficiaries by 2030.
#Trending
MA enrollees made up 35% of all Medicare beneficiaries in 2018 and now make up 44%. MA is attractive to both payers and patients: insurers make a lot of money per patient (over $1,000/patient/month), and beneficiaries get extra health benefits not covered by Original Medicare like vision, hearing and dental health. The writing is on the wall: The MA market is hot and is growing fast.
Record-breaking ACA Marketplace Enrollment
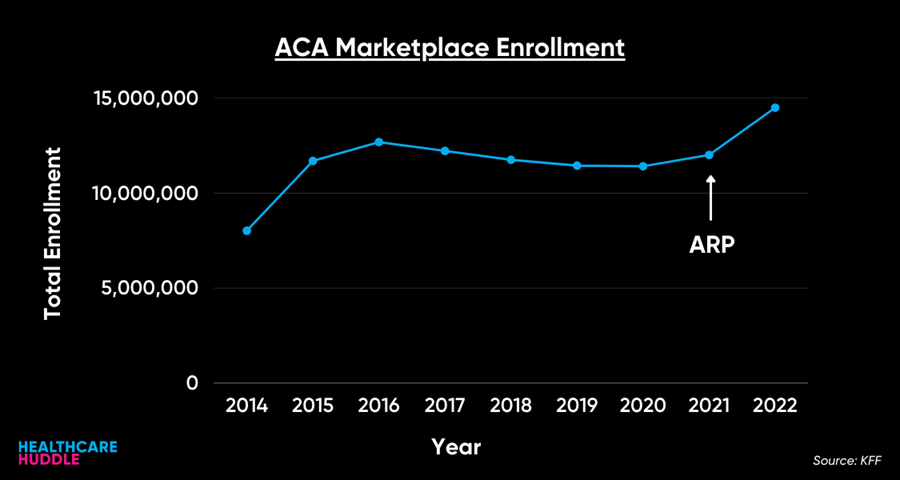
14.5M Americans signed up for health insurance during open enrollment for the Affordable Care Act Marketplace, a 21% increase from 2021. Additionally, 3M people are newly insured, up 17% from last year.
Policy
The No Surprise Billing Act is Live
The No Surprise Billing Act (NSA) is in full swing to protect patients from high medical charges from out-of-network providers.
Surprise medical bills occur when a patient with private insurance receives care from providers or hospitals they did not choose who are out-of-network. The patient’s insurance typically pays less than the full charges (which happens over 75% of the time) and the out-of-network provider sends the patient a hefty bill covering the remainder of the charges. Surprise billing occurs in 20% of emergency room visits and 10% of surgeries that have out-of-network anesthesiologists.
The Fate of Telehealth
Congress plans to extend telehealth flexibilities made during the pandemic for up to five months after the public health emergency ends. These flexibilities include:
- Coverage for telehealth visits, including some audio-only, regardless of the patient’s location relative to the healthcare provider. Before, coverage was limited only to beneficiaries in rural areas who were required to travel to a healthcare facility like an FQHC to have the virtual visit with a doctor who was in another location (seems pointless, I know).
- Provider reimbursement for virtual visits that take place from the patient’s home or medical facilities.
- Delay the requirement that Medicare beneficiaries who use virtual mental healthcare see their mental health provider within six months of the telehealth visit.
Public Health
How Moderna is Advancing Global Health
Moderna released its new global health strategy to accelerate its mRNA technology to prevent infectious diseases worldwide, not just Covid-19.
The Deets
Moderna’s new global health initiative spans four areas:
- Advance mRNA vaccines to target 15 pathogens that pose the biggest threats to global health, including HIV, Zika, TB and Malaria, by 2025.
- Launch mRNA Access, allowing researchers worldwide to use Moderna’s mRNA technology to explore new vaccine designs in preparation for Disease X (whatever that may be).
- Patent pledge to never enforce patent protections on the company’s mRNA technology for the 92 low- and middle-income countries identified by the COVAX initiative (link). Moderna will enforce patent protections for everyone else, citing that vaccine supply is no longer a barrier.
- Establish an mRNA manufacturing facility in Kenya to produce 500 million doses of vaccines each year.
Medicine
The First BRCA-Targeting Breast Cancer Drug
The FDA approved the first and only breast cancer drug Lynparza, which targets BRCA mutations. The drug, made by AstraZeneca and Merck, may reshape the role of BRCA testing in patients with breast cancer.
The FDA green-lighted Lynparza after clinical trial results showed a 42% reduction in the risk of invasive breast cancer recurrence, secondary cancer or death in patients on Lynparza vs. placebo at around 2.5 years follow up. The most recent results show a 32% reduction in death vs. placebo—quite promising. Lynparza is a PARP inhibitor and works by damaging the DNA strands in tumor cells, causing cell death.